Chest congestion can be an uncomfortable and frustrating symptom, often linked to allergies, infections, or respiratory conditions. While many associate seasonal allergies with sneezing and nasal congestion, they can also cause chest congestion allergies. This condition can lead to breathing difficulties and discomfort, making it crucial to understand its causes and find effective relief.
What Causes Chest Congestion from Allergies?
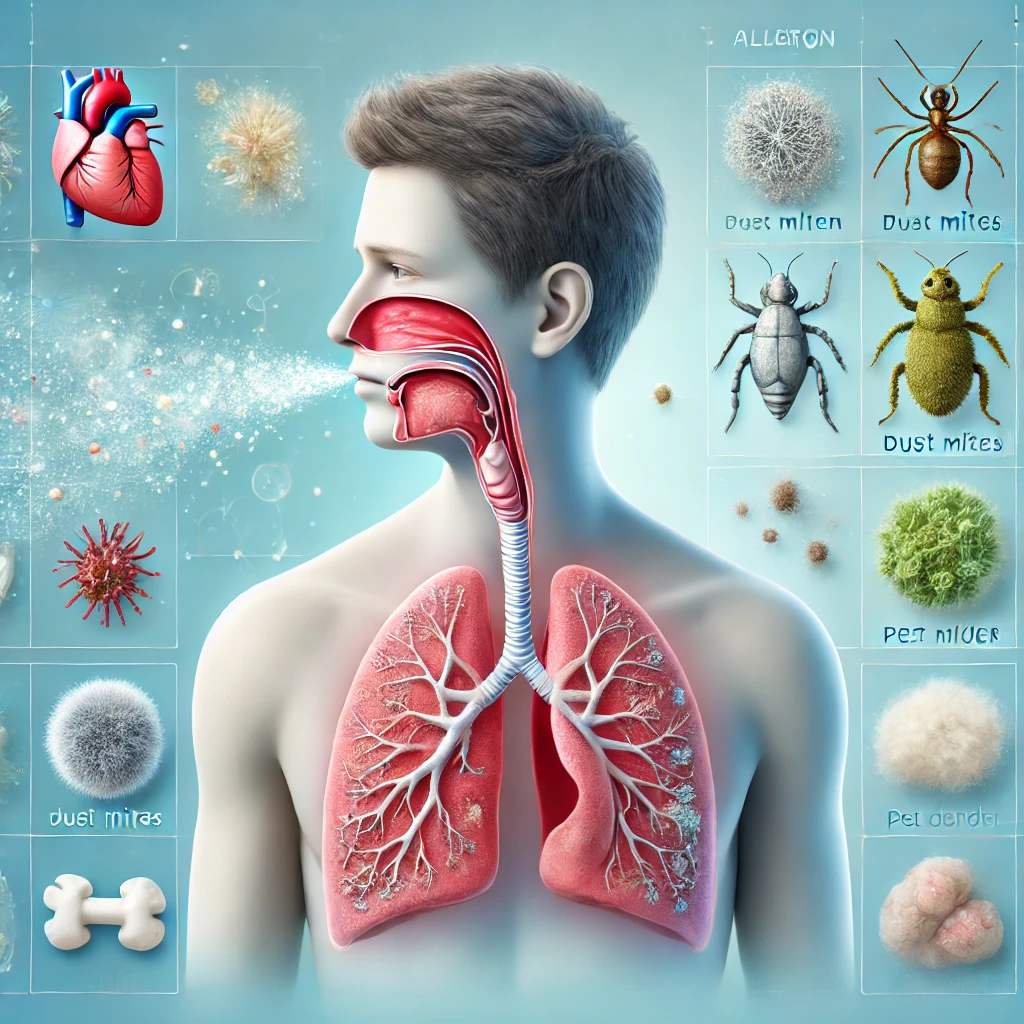
Allergies occur when the immune system overreacts to harmless substances like pollen, dust mites, pet dander, or mold. When allergens enter the respiratory system, the body releases histamines, which trigger inflammation and excessive mucus production. This response can lead to a buildup of mucus in the airways, causing congestion, coughing, and a tight feeling in the chest.
Common Allergens That Can Cause Chest Congestion
- Pollen – A major trigger for seasonal allergies, especially in spring and fall.
- Dust Mites – Microscopic organisms that thrive in bedding, carpets, and upholstery.
- Pet Dander – Proteins found in animal skin cells, saliva, and urine that can cause allergic reactions.
- Mold Spores – Found in damp environments, mold can trigger respiratory issues.
- Airborne Irritants – Smoke, strong odors, and pollution can worsen allergy-related congestion.
Symptoms of Chest Congestion Due to Allergies
Recognizing the symptoms of allergy-related chest congestion is essential for effective management. These symptoms include:
- A persistent cough, often worse at night or early morning
- Wheezing or a whistling sound when breathing
- Shortness of breath, especially after exposure to allergens
- A heavy or tight sensation in the chest
- Postnasal drip leading to throat irritation
- Increased mucus production, causing a clogged or heavy feeling in the lungs
- Fatigue due to reduced oxygen intake and disrupted sleep
While these symptoms may resemble those of respiratory infections, they usually occur in response to allergen exposure rather than bacteria or viruses.
How to Relieve Allergy-Related Chest Congestion
If you experience chest congestion allergies, managing your environment and adopting the right treatment plan can provide relief. Here are some effective strategies:
1. Identify and Avoid Triggers
Limiting exposure to allergens is the first step in preventing chest congestion. Simple changes, such as using air purifiers, washing bedding frequently, and keeping windows closed during high pollen seasons, can make a significant difference.
- Use hypoallergenic pillowcases and mattress covers to reduce exposure to dust mites.
- Keep pets out of the bedroom if you are allergic to pet dander.
- Avoid outdoor activities during peak pollen hours, usually in the morning and evening.
- Maintain indoor humidity levels below 50% to prevent mold growth.
2. Use Over-the-Counter Medications
Several medications can help alleviate allergy-related chest congestion, including:
- Antihistamines – Reduce the body’s allergic reaction and minimize mucus production.
- Decongestants – Help clear nasal passages and reduce swelling in airways.
- Nasal Corticosteroids – Reduce inflammation in the nasal passages and ease postnasal drip.
- Expectorants – Help loosen mucus so it can be expelled more easily through coughing.
However, it’s best to consult a healthcare professional before using these medications long-term, as some may cause side effects.
3. Try Home Remedies for Natural Relief
Home remedies can provide additional relief from allergy-related chest congestion:
- Steam Inhalation – Inhaling steam from hot water or a humidifier can loosen mucus and soothe irritated airways. Adding essential oils like eucalyptus can enhance the effect.
- Saline Nasal Rinse – Using a saline solution can flush out allergens from the nasal passages, reducing congestion.
- Honey and Ginger Tea – Honey has natural antibacterial properties, while ginger helps reduce inflammation and clear airways.
- Hydration – Drinking plenty of fluids helps thin mucus, making it easier to clear from the airways.
4. Consider Allergy Immunotherapy
For individuals with persistent or severe allergies, allergy shots or sublingual immunotherapy (under-the-tongue tablets) can help the immune system build tolerance to specific allergens over time. This long-term treatment can significantly reduce allergy symptoms, including congestion.
5. Seek Professional Help
If your symptoms persist or worsen, seeking medical advice is crucial. An allergy specialist or pulmonologist can provide tailored treatments, including:
- Allergy Testing – Identifying specific allergens to create a personalized management plan.
- Prescription Medications – Stronger treatments, such as leukotriene inhibitors or inhaled steroids, may be necessary for severe cases.
- Breathing Treatments – In some cases, nebulizers or bronchodilators may be recommended to open airways.
Lifestyle Changes to Prevent Allergy-Related Chest Congestion
Making small lifestyle adjustments can significantly reduce the occurrence of chest congestion due to allergies. Consider the following:
- Maintain a Clean Living Space – Regular cleaning reduces the presence of dust, mold, and pet dander.
- Shower Before Bed – This prevents pollen and other allergens from transferring to bedding.
- Use HEPA Filters – High-efficiency particulate air (HEPA) filters trap allergens, improving indoor air quality.
- Exercise Indoors on High-Pollen Days – Outdoor exercise during peak allergy season can increase exposure to allergens.
When to See a Doctor
Although allergies can be managed at home, severe or persistent chest congestion should not be ignored. If you experience:
- Extreme difficulty in breathing
- Persistent wheezing
- A chronic cough lasting more than three weeks
- Symptoms that interfere with daily activities
… it’s time to consult a specialist.
At Interstate Pulmonary, experienced medical professionals can help diagnose and treat respiratory conditions caused by allergies. If you’re struggling with allergy-related chest congestion, schedule an appointment today. Contact us here for expert guidance and personalized treatment.
Conclusion
Allergy-induced chest congestion can be distressing, but with the right approach, relief is achievable. Identifying triggers, using medications when necessary, and seeking medical advice can help you breathe easier. Managing chest congestion allergies effectively ensures a better quality of life, especially for those prone to seasonal allergies.
If your symptoms persist, don’t hesitate to seek professional assistance for a tailored treatment plan. By understanding the link between allergies and chest congestion, you can take proactive steps to minimize discomfort and improve respiratory health.